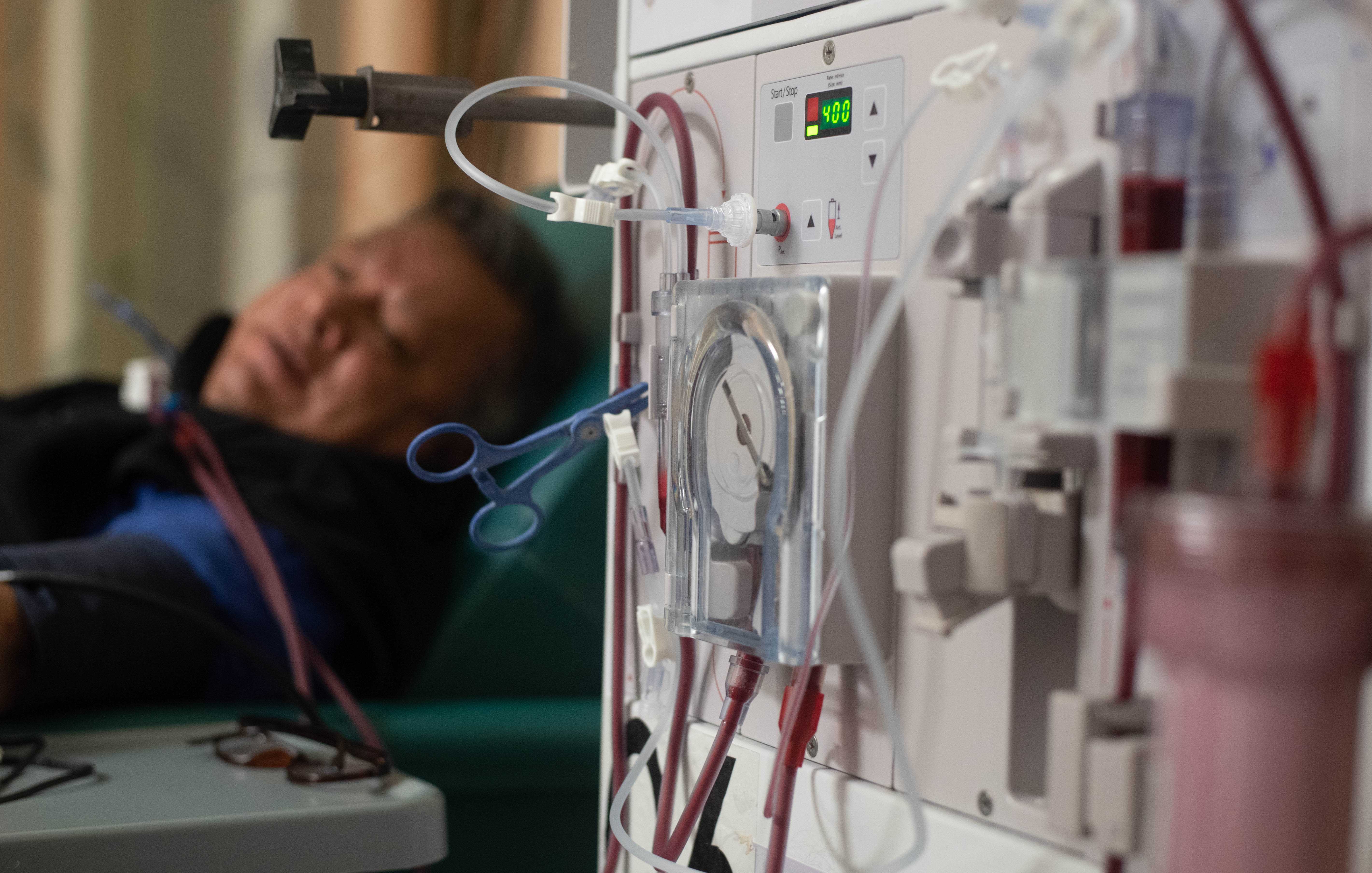
At 5 a.m., three days a week, in a North Jersey suburb, a 59-year-old former warehouse worker whose kidneys are failing jokes his way through the dialysis that keeps him alive. Beneath the harsh glare of fluorescent lights, he props himself up next to the gray machine that filters toxins from his blood. A nurse inserts two needles into a deep purple injection site, swollen to the size of a tennis ball, on his upper right arm.
Daniel, short, grey-haired and heavyset, is all smiles and chatter as the four-and-a-half hour process begins. Even as he starts to feel weak and his lower arm turns numb, he manages to distract himself from the pain by watching early morning TV and listening to Grupo Audaz, an upbeat band from his hometown of Veracruz in southern Mexico. But on bad days, Daniel said, he gets cramps that would make “even Superman cry.”
After years of treatment, he’s learned to cope. “At the beginning,” he said, “it was a battle between me and the technology. But then I understood that this machine is giving me life.”
As grueling as it is, Daniel, a husband and father of two who has lived in this country for three decades, feels lucky to have access to treatment at all. He’s an undocumented immigrant, who Documented is identifying only by his first name because his care could be in jeopardy if authorities found out about it.
But Daniel doesn’t think about such risks. Instead, he focuses on the day-to-day. “People look at you like, ‘Oh, poor you,’” he said. “No, you have to be active. I already have this disease. I have to live each day as if it is the last.”
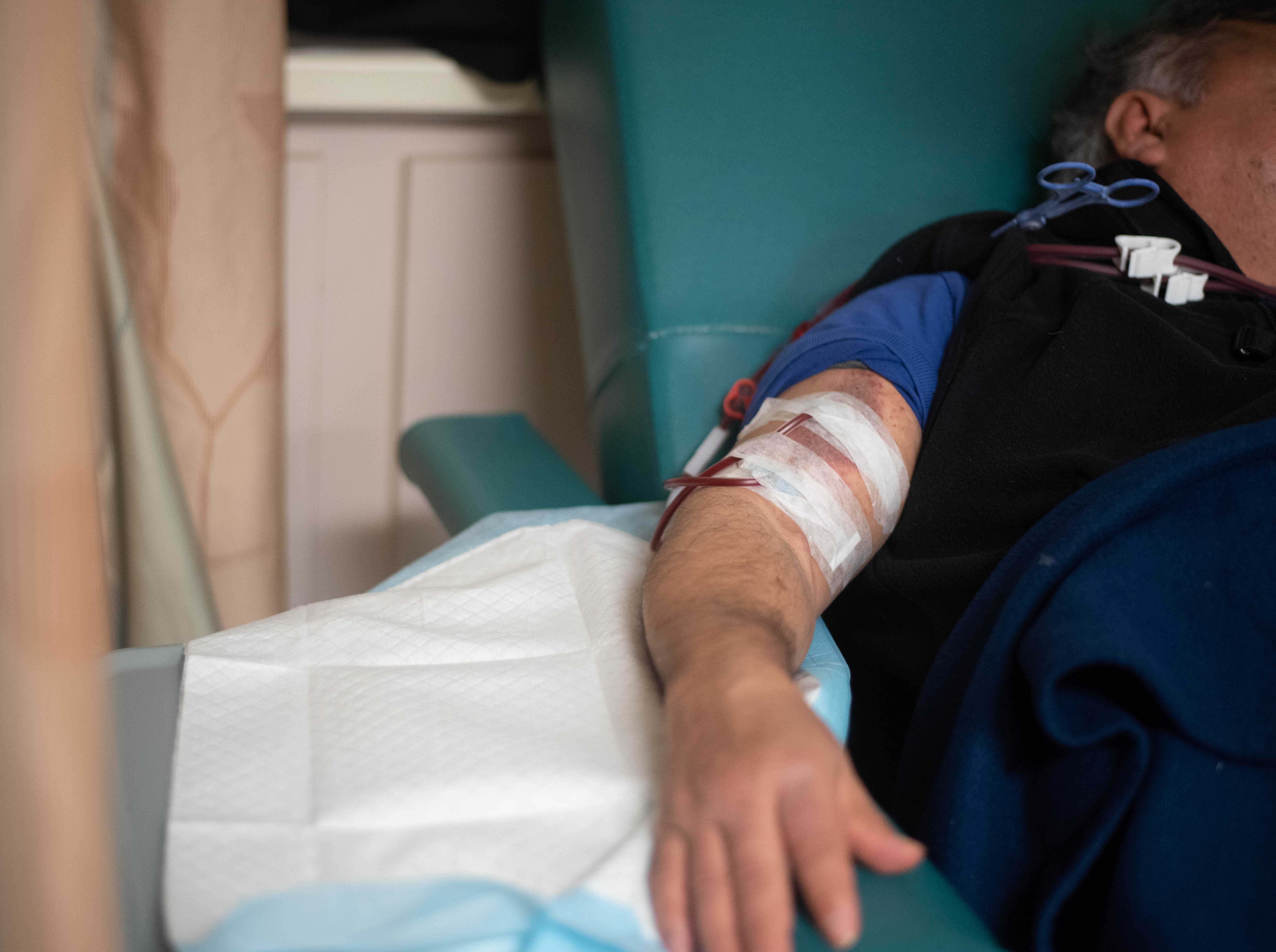
It’s long been difficult for undocumented immigrants suffering end-stage renal failure to get the medical care they need in New Jersey. But now, according to immigrant advocates and social workers, it’s becoming harder. They say that the patchwork system cobbled together to serve undocumented immigrants over the last decade, which requires the state’s 186 dialysis clinics to provide 3.5 percent of their services to patients who need charity care, is at capacity.
The situation has left patient advocates and hospitals pushing clinics to expand the number of uncompensated cases they’ll take. Clinics are turning needy patients away. And hospitals treating the overflow complain the costly procedures are a drain on their resources.
Christopher Brown oversees the quality of care provided by New Jersey’s outpatient dialysis clinics for the Department of Health and Human Services, which has put him in the middle of this burgeoning crisis. “This is not sustainable,” he said. “We need a more long-term solution.”
Brown and his team often help connect uninsured patients with clinics willing to provide free care for them. For years, he said, he’s not had much trouble. In March, however, he got a call from a North Jersey hospital asking for help placing seven undocumented patients. And for the first time, every clinic he called turned him down, saying they had already met or exceeded the 3.5 percent of charity cases that are required.
Brown didn’t believe them, and began to crunch the numbers. Using a database that his office maintains of all patients registered in New Jersey dialysis clinics, he identified those receiving treatment who did not have Social Security numbers. They accounted for 3.9 percent of the entire patient load – well beyond the legal mandate.
“Honestly, until this seven patient issue came up, we were not even aware of what the percentages were,” Brown said. Running the numbers showed them “how big the problem really was. We never really appreciated how many undocumented patients were receiving uncompensated care until we did that.”
The seven patients, Brown said, came here from countries in the Middle East and Eastern Europe because they did not have access to care in their home countries. A month after their arrival, the outlook for their care in New Jersey is uncertain. The hospital treating them has made clear they don’t want to do so indefinitely. Brown said he’s found a clinic that might be willing to take one of the seven. As for the other six, Brown is “brainstorming.”
Although he’s sympathetic to the hospital’s financial concerns, he said, “I’m also sensitive to the patients that are probably going to die if they are sent back to their home countries.”
The number of those patients in need, he said, is growing. But he has no idea how much. “We’re a little bit frustrated right now,” he said.
To get a better handle on the scope of the problem, Brown has partnered with the New Jersey Hospital Association to get a complete count of undocumented patients being treated in all of the state’s hospitals and clinics. Once they know that number, they would be in a stronger position to push for reforms that would provide consistent care to them.

The landscape of care looks entirely different just across the Hudson River in New York. Authorities there expanded the state’s Medicaid program to cover dialysis for undocumented immigrants. Ten other states across the country, including most recently Colorado, have enacted similar measures.
This summer, New York City plans to offer municipal health insurance for all low-income New Yorkers, including those who are undocumented, so they can receive basic care. The program, called NYC Care, will start in the Bronx and is expected to be in place throughout the city by 2021.
Some social workers and health authorities in New Jersey wonder why their state doesn’t do the same. Iya Bekondo-Granatella is the executive director of The Iya Foundation, a nonprofit that advocates for kidney health and works extensively within New Jersey’s African immigrant community to help connect them with services. Like Brown, she too has found it hard to find clinics or hospitals that will provide regular dialysis for her clients. She said that some wait until they’re near death before turning to an emergency room for help, and she knows multiple people who depend on emergency dialysis to stay alive.
“Sometimes, that’s the extent to which they have to go,” she said. “The hospital can’t turn their back on them.”
Other patient advocates think every state could do better, and save taxpayer dollars, by providing preventive care so that undocumented immigrants don’t have to rely on dialysis in the first place, like NYC Care is planning to do starting in the summer. Mukta Baweja, a nephrologist and national health policy advocate in New York City, says the growing demand for dialysis is a “direct consequence” of where the real problem lays. The cost of basic healthcare is financially crippling for low-income patients across the country, but without it, people with chronic conditions like diabetes deteriorate to a point where their kidneys fail and they need dialysis.
Baweja said she’s seen such cases time and again. She treated one young undocumented mother who had no insurance and rationed her kidney medications, because she could not afford both the medication and groceries for her family. “If you think about it, she’s killing herself slowly to save her children,” Baweja said.
So many of these kinds of patients, she said, could be cured with kidney transplants. But if dialysis is hard to get, transplants are near impossible. Even when patients have compatible donors, hospitals are often unwilling to take their cases because they either don’t have insurance, or lack the ability to pay privately for the procedures and the years of medications needed afterward.
Bekondo-Granatella speaks about this dilemma from experience. She came to New Jersey from Cameroon 19 years ago as an undocumented teenager dying from kidney disease. A hospital provided her dialysis for years, through charity care. Then in 2005, her church and school raised $33,000 for surgery to transplant a kidney from her mother. It changed her life. She became a citizen, earned two master’s degrees and started her own foundation that arranges for low-income kidney patients in New Jersey and Cameroon to receive dialysis and transplants.
“What we’ve been fighting for is to make transplants more accessible,” she said. “Transplants are way cheaper in the long run than dialysis treatments.”
Medical professionals say it’s one thing to give uninsured, low-income patients new kidneys, but if they can’t afford the monthly post-surgery appointments and medications, the organ will die. Thomas Lepetich has worked as a dialysis social worker all over New Jersey for 33 years. He describes the transplant process like buying a house.
“Even if somebody puts the downpayment down for you, if you don’t have the money for the monthly payment, your house is going to go into foreclosure,” Lepetich said. It’s a system stacked against low-income patients. Whether their “families came over on the Mayflower” or not, he said. “It sucks. It sucks even more if you’re undocumented.”
Daniel knows this predicament well. He had a transplant in 2003, 11 months after what seemed like a case of indigestion turned out to be a condition that not only forced him to leave his job, but also nearly killed him. The donor was one of his nephews. The hospital agreed to give him the transplant, he says, because of his “many angels.” But to hear him talk about it, it sounds more like a determined family campaign, led by Daniel and his wife, Elizabeth, who knocked on one authority’s door after another. Someone in the local government sent him to someone at the Mexican consulate who sent him to an office at the Social Security Administration, where he got a card that allowed him to be enrolled in Medicare and get the surgery.
The new kidney served him well for 15 years, even allowing him to go back to work for a time. But as most transplanted kidneys do at that point, Daniel’s gave out. In July 2018 he was back in dialysis, thanks again to the Social Security card. Hospitals, however, refuse to allow him to get a second transplant, saying he doesn’t have insurance or the money to pay for the surgery.
For now, he and his family are resigned to the thrice-weekly dialysis treatments. Sitting in their kitchen, cluttered with waiting dishes, bright orange pill bottles and pictures of their seven-year-old granddaughter, Daniel and Elizabeth talk about how far they’ve come. Since Daniel started dialysis the first time, he stopped being the family’s breadwinner. For a while, Daniel said, he even lost his will to live. But Elizabeth wouldn’t hear of it, and took charge of things for a while. “I would marry her all over again,” Daniel smiled.
Today, Elizabeth said, age has mellowed him. He’s less “rebellious” about going to dialysis. Elizabeth prays, against the odds, that her husband will luck into another transplant – their son is willing to give one of his kidneys if and when they find a hospital willing to do the surgery. And then, they hope, they can retire to South Carolina. The coast there reminds them of the beaches on the Gulf of Mexico, where Daniel was born.
One uphill battle after another has taught Elizabeth never to say never. “God always sends angels, don’t you think?”